Case Report - (2022) Volume 9, Issue 3
Scrotal gunshot injury resulting in a bilateral orchiectomy: A case report
Thomas L. Haupt1*, Vanessa Aponte1, Abhishek Tippabhatl1, Murad Alfaqih1 and Pamela Coleman2Abstract
Scrotal and testicular injuries are rare and most commonly due to penetrating trauma by firearms. Management generally involves prompt surgical exploration and repair depending on the extent of the lesions. Moreover, if the damaged testis is nonviable, an orchiectomy may be recommended to avoid complications. There is currently limited documentation describing cases of a bilateral orchiectomy to manage penetrating scrotal trauma. Therefore, we report a case of a young male with a single gunshot wound to the scrotum that ultimately resulted in the loss of both testicles. The use of doppler ultrasound confirmed the suspicion of ischemic orchitis, ultimately accelerating and guiding surgical exploration.
Keywords
Scrotum, trauma, testicle, orchiectomy, urology, gunshot wound
Introduction
Scrotal and testicular injuries are most commonly due to penetrating trauma by firearm and account for <1% of trauma-related injuries [1]. Although generally not life-threatening, quick diagnosis and management are critical to avoid complications such as infection, infertility, and testicular loss [1]. Management generally involves prompt debridement and surgical repair depending on the extent of the lesions. However, after thorough irrigation and testicular examination, an orchiectomy, defined as a surgical procedure to remove one or both testes [2], maybe recommended if reconstruction of the damaged testis is determined to be nonviable [3]. A recent retrospective review identified that an orchiectomy is performed in roughly 50% of testicular injuries due to penetrating trauma by firearm [4]. However, there is currently limited documentation describing cases of a bilateral orchiectomy to manage penetrating scrotal trauma [5]. Herein, we report the case of a young patient with a single gunshot wound by a handgun resulting in a bilateral testicular loss.
Case Presentation
The patient is a 15-year-old male brought to the emergency department with a 1-hour history of a single gunshot wound to the right medial thigh and scrotum (Fig 1). The patient stated he was being robbed. On arrival, the scrotum was open, and both testicles were avulsed. Additionally, there was an open thigh wound on the right extremity, irregular black skin discoloration on the right palm resembling gunpowder, and a laceration of the distal fourth and fifth digits on the right hand (Fig 2). Shortly after arrival at the emergency department, X-rays of the lower pelvis of the patient were obtained. They showed multiple fragmented debris overlying the right upper thigh and scrotal area (Fig 3). Subsequently, the patient underwent a scrotal ultrasound with a doppler that demonstrated the absence of significant blood flow to either the right or left testes. The time from the onset of the gunshot wound to the time of scrotal ultrasound was approximately 2.5 hours.
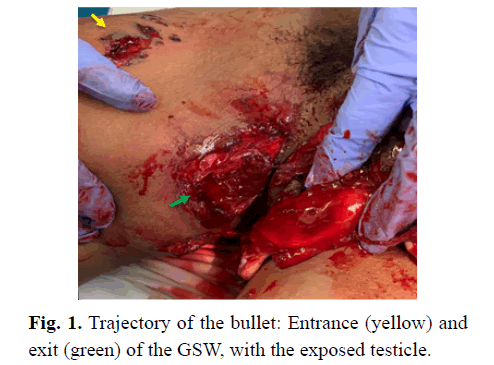
Figure 1: Trajectory of the bullet: Entrance (yellow) and exit (green) of the GSW, with the exposed testicle.
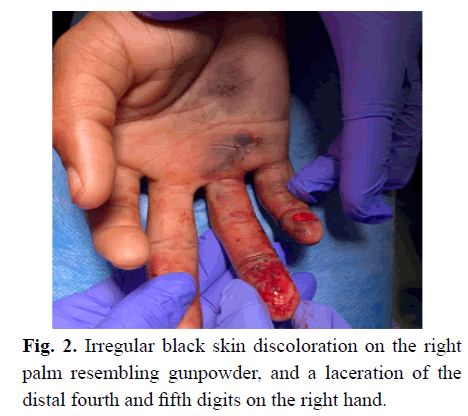
Figure 2: Irregular black skin discoloration on the right palm resembling gunpowder, and a laceration of the distal fourth and fifth digits on the right hand.
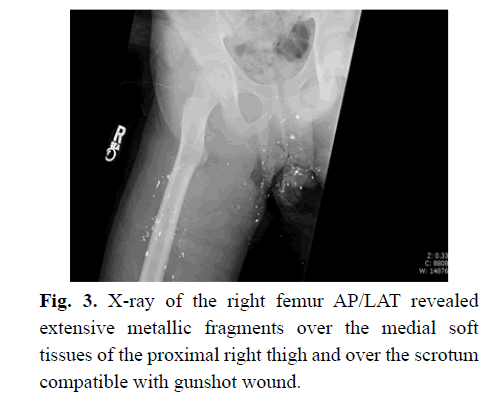
Figure 3: X-ray of the right femur AP/LAT revealed extensive metallic fragments over the medial soft tissues of the proximal right thigh and over the scrotum compatible with gunshot wound.
Soon after, the decision to take the patient to the operating room was made, and upon surgical exploration, both spermatic cords were almost wholly avulsed from the proximal portion (Figs 4 and 5). Further examination showed diffuse foreign body debris involving the dartos fascia, tunica vaginalis, and spermatic cords. The testicles were exposed; no tunica albuginea was identifiable, and the epididymis was fractured from the superior pole of the testes (Fig 6). After meticulous exploration, both testicles were determined to be nonviable, and a bilateral total orchiectomy was performed. The penis was able to be salvaged. The area was irrigated, and a drain was placed exiting a separate incision of the left hemiscrotum. The scrotal wall was reconstructed, and the underlying dartos fascia was closed.
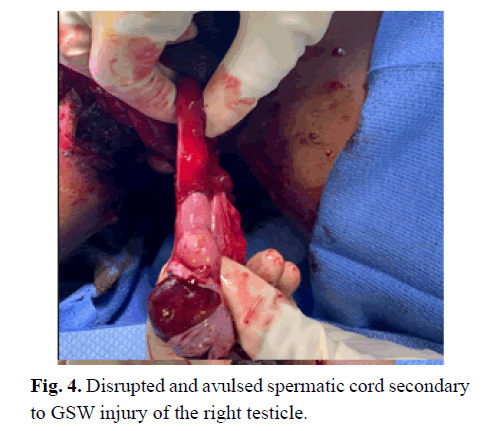
Figure 4: Disrupted and avulsed spermatic cord secondary to GSW injury of the right testicle.
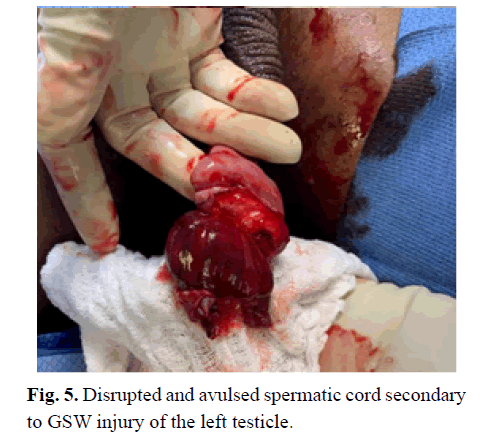
Figure 5: Disrupted and avulsed spermatic cord secondary to GSW injury of the left testicle.
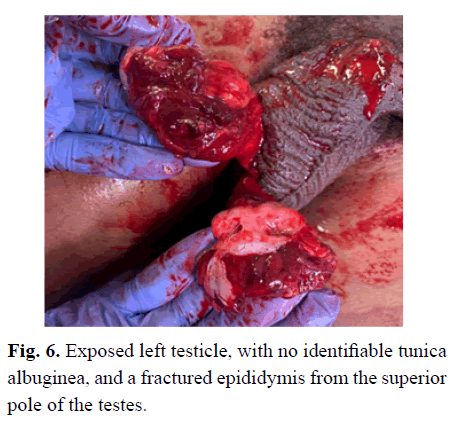
Figure 6: Exposed left testicle, with no identifiable tunica albuginea, and a fractured epididymis from the superior pole of the testes.
Postoperative care involved medical management of primary hypogonadism and two operative procedures performed by plastic surgery for the right thigh injury. The testosterone level after the injury but before the bilateral orchiectomy was approximately 78 ng/ dL. Subsequently, on postoperative day one, the testosterone level dropped to 14 ng/dL, and the FSH and LH levels were recorded to be 5.83 IU/L and 2.91 IU/L, respectively. Twelve days after the bilateral orchiectomies, the testosterone level was recorded as <10 ng/dL, and the FSH and LH levels were recorded to be 53.50 IU/L and 27.97 IU/L, respectively. The patient was followed up with endocrine and plastic surgery one week later.
Results and Discussion
MThis case is compelling due to the unique features of the patient’s age, mechanism of injury, and that single gunshot wound to the scrotum ended in bilateral testicular loss. In previous literature, the median age of the reported patients with testicular and scrotal trauma is approximately 31 years [1]. In contrast, we report a 15-year-old. This atypical age is near the end of puberty, and this injury precludes a lifetime of numerous endocrine consequences due to a deficit of endogenous testosterone.
Additionally, a unique aspect of this case is that the patient did not fully explain the mechanism of the gun injury. Upon questioning, the patient stated that an assailant was robbing him in front of him. However, given the trajectory of the bullet and the gun powder- like discoloration and lesions on the patient’s hand, we determined that the injury was most likely an accidental discharge, most often described as self-inflicted [6]. Previous reports of self-inflicted testicular injuries are limited and considered very rare [6,7]. A prior case series by Ukpong et al. reported a patient who sustained a self- inflicted bilateral testicular injury following accidental discharges from a handgun kept in his pants pockets [6]. However, unlike in our case, this patient’s testes were salvaged by repair after thorough debridement. In summary, scrotal and testicular injuries are rare and only account for <1% of trauma-related injuries [1]. A bilateral testicular injury from a single gunshot wound is even rarer [5,8]. In a previous study, Sinham et al. reported that out of 97 patients with genital gunshot injuries, only 6 patients’ experienced bilateral testicular injuries [4]. The difference in outcome between our case and previous self-inflicted testicular injuries makes our case even rarer in that our patient lost both testicles.
Moreover, in this case, the utilization of ultrasound confirmed the suspicion of tunica albuginea rupture and absent blood flow to both testes. This finding was subsequently confirmed during surgical exploration of the scrotum. Unfortunately, the tunica albuginea was hardly identifiable, and both testicles were determined to be nonviable, leading to the bilateral orchidectomy being performed. The American Urology Association (AUA) clinical recommendations for blunt scrotal injuries entail quick imaging modalities such as doppler ultrasound to assess testicular damage, while penetrating injuries warrant urgent surgical exploration due to the increased risk of testicular rupture [3]. Furthermore, previous literature recommends that scrotal ultrasonography only be used for patients with a low index of suspicion due to intact dartos fascia, as the sensitivity of scrotal ultrasound has been demonstrated to be limited [4,9,10]. However, in this case, the magnitude of the injury was so severe that the Doppler ultrasound confirmed the suspicion of absent blood flow to the testes and loss of structural integrity, which ultimately helped in the navigation of surgical exploration rather than the utilization of Doppler ultrasound as a screening tool for surgical exploration
Conclusion
In summary, we report a case of a young male patient with a self-inflicted single gunshot wound to the scrotum that ultimately resulted in bilateral testicular loss. This presentation is unique because a single gunshot wound interrupted both testicular blood flows and resulted in a bilateral orchiectomy. In addition, the use of Doppler ultrasound confirmed the suspicion of the absence of blood flow to the testes, ultimately accelerating and guiding surgical exploration.
Conflict of Interest
The authors declare no conflicts of interest.
Funding
The authors received no financial support for this work.
Consent
Patient consent form has been obtained.
References
- Grigorian A, Livingston JK, Schubl SD, et al. National analysis of testicular and scrotal trauma in the USA. Res Rep Urol. 2018;10:51.
[Cross Ref] [Google Scholar] [PubMed]
- Okoye E, Saikali SW. Orchiectomy. Treasure Island. 2022.
[Google Scholar] [PubMed]
- Morey AF, Brandes S, Dugi DD, et al. Urotrauma: AUA guideline. J Urol. 2014; 192(2):327-35.
[Cross Ref] [Google Scholar] [PubMed]
- Simhan J, Rothman J, Canter D, et al. Gunshot wounds to the scrotum: a large single-institutional 20-year experience. BJU international. 2011;109(11):1704-7.
[Cross Ref] [Google Scholar] [PubMed]
- Cass AS, Ferrara L, Wolpert J, et al. Bilateral testicular injury from external trauma. J Urol. 1988;140(6):1435-6.
[Cross Ref] [Google Scholar] [PubMed]
- Ukpong AE, Akaiso OE, Udo EA, et al. Scrotal self-inflicted gunshot injuries: report of two consecutive cases and literature review. Afr J Urol. 2021;27(1):1-5.
- Obi AO, Ulebe AO, Nnadozie UU, et al. Self-inflicted gunshot injury to the external genitalia: a case report and review of literature. Afr J Urol. 202;27(1):1-5.
- Gomez RG, Castanheira AC, McAninch JW. Gunshot wounds to the male external genitalia. J Urol. 1993;150(4):1147-9.
[Cross Ref] [Google Scholar] [PubMed]
- Powers R, Hurley S, Park E, et al. Usefulness of preoperative ultrasound for the evaluation of testicular rupture in the setting of scrotal gunshot wounds. J Urol. 2018;199(6):1546-51.
[Cross Ref] [Google Scholar] [PubMed]
- Corrales JG, Corbel L, Cipolla B, et al. Accuracy of ultrasound diagnosis after blunt testicular trauma. J Urol. 1993;150(6):1834-6.
[Cross Ref] [Google Scholar] [PubMed]
Author Info
Thomas L. Haupt1*, Vanessa Aponte1, Abhishek Tippabhatl1, Murad Alfaqih1 and Pamela Coleman22Department of Surgery, Howard University Hospital, Washington DC, USA
Received: 05-Apr-2022, Manuscript No. PUCR-22- 59681; , Pre QC No. PUCR -22-59681 (PQ); Editor assigned: 08-Apr-2022, Pre QC No. PUCR -22-59681 (PQ); Reviewed: 29-Apr-2022, QC No. PUCR-22-59681; Revised: 06-May-2022, Manuscript No. PUCR-22-59681 (R); Published: 13-May-2022, DOI: 10.14534/j-pucr.2022267579
Copyright: This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
